Scalp folliculitis is one of the most underreported scalp conditions in Malaysia — not because it is rare, but because patients frequently mistake it for scalp acne, treat it incorrectly, and allow an infection that responds well to early intervention to progress into a chronic or scarring condition. The scalp's dense follicular architecture, combined with Malaysia's climate, creates ideal conditions for follicle infection across all three of its primary types: bacterial, fungal, and eosinophilic.
The single most consequential decision in folliculitis management is identifying the type before selecting treatment. Bacterial folliculitis requires antibacterials. Fungal (Pityrosporum) folliculitis requires antifungals. Eosinophilic folliculitis requires immunomodulatory management. Applying an antifungal to bacterial folliculitis does not simply fail — it allows bacterial progression while a false-negative treatment response delays referral.
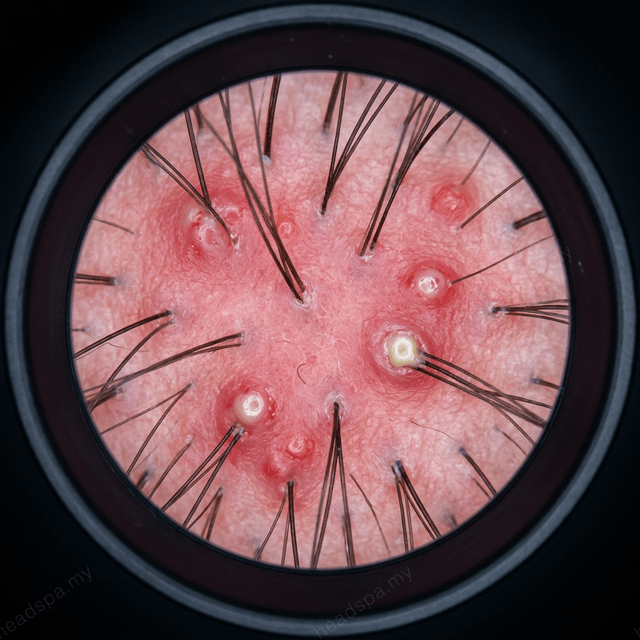
Three Types of Scalp Folliculitis
| Type | Causative Agent | Appearance | Key Triggers | Primary Treatment | |---|---|---|---|---| | Bacterial (most common) | *Staphylococcus aureus*; less commonly gram-negative organisms | Tender pustules, erythematous papule surrounding the hair, yellow crust on resolution | Heat, humidity, sweat, shaved scalp, shared hair tools, microtrauma from tight hairstyles | Topical mupirocin or clindamycin; chlorhexidine wash; oral antibiotics (flucloxacillin, doxycycline) for moderate-severe; decolonisation for recurrent cases | | Fungal / Pityrosporum | *Malassezia furfur* (Pityrosporum ovale) | Monomorphic, pruritic papulopustules; often follicular; perioral or truncal extension common; confused with bacterial type | Humid climate, immunosuppression, prolonged antibiotic use, high sebum output | Topical ketoconazole or selenium sulfide; oral itraconazole or fluconazole for extensive cases; avoid antibiotics (worsen fungal overgrowth) | | Eosinophilic | Immune dysregulation; associated with HIV, immunosuppression | Intensely pruritic urticarial papules; eosinophilia on bloods; does not respond to antibiotics or antifungals | HIV/AIDS, haematological malignancy, immunosuppressive therapy | Systemic treatment — HIV management is primary; topical potent corticosteroids; phototherapy; oral indomethacin |
Why Malaysia's Climate Accelerates Folliculitis
Bacterial folliculitis risk is higher in tropical climates for mechanistically clear reasons. *Staphylococcus aureus*, the primary causative organism, colonises the anterior nares and skin surface of approximately 30% of healthy adults. In a temperate climate, intact skin with a functioning acid mantle provides an effective barrier. In Malaysia's year-round heat and humidity, two failure modes become more frequent.
First, persistent sweating creates sustained surface moisture that softens the stratum corneum, increasing permeability to bacterial penetration. Second, sebum liquefaction at elevated ambient temperatures causes sebum to spread more broadly, providing an enlarged nutritional substrate for skin surface bacteria. Both effects are permanent in Malaysia — there is no cold or dry season to interrupt the cycle.
Communal risk factors relevant to the Malaysian population include shared hair combs and brushes (a culturally common practice in family and social settings), swimming pools where the water-to-skin contact risk is high, and barbershop equipment with insufficient sterilisation between clients.
Tight Hairstyles and Mechanical Follicular Trauma
Tight braiding, high-tension ponytails, and the mechanical friction created by non-breathable headwear all generate micro-trauma at the follicle base. The damaged follicular epithelium provides an entry point for surface bacteria. This mechanism — traction-mediated barrier disruption followed by bacterial invasion — is distinct from primary infection and requires addressing the mechanical factor alongside the antimicrobial treatment to prevent recurrence.
For Muslimah clients wearing hijab, the combined effect of fabric friction at the hairline, elevated scalp temperature and humidity, and any tight-fitting undercap creates a microenvironment with measurably elevated folliculitis risk. TTE Elephant's team provides specific clinical guidance for this population, including undercap material recommendations and scalp hygiene protocols compatible with daily hijab wearing. Our [KL clinic](/headspa-kl) and [JB clinic](/headspa-jb) are set up to manage these cases.
Why Folliculitis Becomes Chronic: Biofilm and Nasal Carriage
A subset of patients experience recurrent bacterial folliculitis — lesions that resolve with treatment but return within weeks to months. Two mechanisms explain most chronic cases.
The first is *S. aureus* nasal carriage. Approximately 30% of adults persistently carry *S. aureus* in the anterior nares and auto-innoculate their skin from this reservoir. Treating scalp lesions without addressing nasal carriage is treating the symptom without its source; recurrence is virtually certain. Nasal decolonisation with mupirocin nasal ointment is a standard component of chronic folliculitis management but requires dermatologist oversight.
The second is biofilm formation. *S. aureus* is a proficient biofilm producer — it can establish a surface-adherent community encased in a polysaccharide matrix that is significantly more resistant to antibiotics than planktonic bacteria. Biofilm-embedded folliculitis tends to respond initially to antibiotic courses but recurs as the biofilm re-establishes. This pattern — treatment response followed by recurrence — is a clinical signal for biofilm involvement and warrants dermatology referral for extended or combination antibiotic protocols.
The Scarring Alopecia Risk
Untreated or inadequately treated folliculitis can progress from superficial (within the follicular infundibulum) to deep (involving the follicular isthmus and hair bulge). Deep folliculitis — folliculitis decalvans in its destructive variant — destroys the follicle permanently. The hair follicle does not regenerate after destruction; the result is a patch of scarring alopecia that is irreversible without surgical intervention.
This is not an outcome reserved for severe or neglected cases. Folliculitis decalvans can develop from undertreated moderate folliculitis in individuals with susceptible immune profiles. Any folliculitis case accompanied by spreading erythema, tufted hairs (multiple hairs emerging from a single enlarged follicle), or progressive hairline recession without active traction should be treated as a dermatological emergency — referral same-day or within 48 hours.
TTE Elephant's Clinical Role
TTE Elephant's trichoscopy assessment can identify folliculitis type and severity at the first consultation. For mild-to-moderate bacterial folliculitis, TTE's protocol includes a chlorhexidine-based scalp treatment, assessment of contributing factors (sebum overproduction, product buildup, mechanical trauma), and structured follow-up. The trichoscopy-guided approach means treatment is matched to the actual pathology, not selected generically.
For cases that exceed the clinical scope of head spa — moderate-severe bacterial infection, any suspected fungal folliculitis, eosinophilic folliculitis, or progressive hair loss — TTE coordinates referral to partner dermatologists in Kuala Lumpur and Johor Bahru. Clients do not need to self-navigate the dermatology system; TTE provides clinical handover with trichoscopy documentation.
Related reading: [Scalp Folliculitis Symptom Profile](/concerns/scalp-folliculitis) | [TTE Elephant Head Spa KL](/headspa-kl) | [TTE Elephant Head Spa JB](/headspa-jb)
---
Frequently Asked Questions
Q: How do I know if my scalp pimples are folliculitis or just regular scalp acne?
A: The key distinction is infection versus occlusion. Scalp folliculitis produces tender, erythematous (red-ringed) pustules that are painful to touch, may feel warm, and can develop crusting as they heal. Regular comedonal scalp acne produces non-tender, non-red plugged follicles or whiteheads without significant surrounding inflammation. If lesions are painful, spreading, or accompanied by any systemic symptoms such as fever, folliculitis is the more likely diagnosis and clinical assessment is appropriate.
Q: Can I go swimming in a public pool if I have scalp folliculitis?
A: Not during an active infection. Pool water, despite chlorination, represents a gram-negative bacterial exposure risk (Pseudomonas aeruginosa, the causative agent of hot tub folliculitis, is chlorine-tolerant at typical pool concentrations). Beyond introducing new organisms, the physical immersion and towelling post-swim causes mechanical disruption to healing pustules. Wait until all active lesions have resolved and the scalp surface is intact before returning to pool swimming. Shower and shampoo immediately after any pool session once cleared, as a preventive measure.
Q: Why does my folliculitis keep coming back even after antibiotic treatment?
A: Recurrent folliculitis despite treatment is most commonly explained by either *Staphylococcus aureus* nasal carriage (you are reinfecting your scalp from your own nasal reservoir) or biofilm formation (bacterial communities that resist antibiotic penetration). Both require dermatologist-managed protocols — nasal swab culture, decolonisation treatment, or combination antibiotic approaches — rather than repeated courses of the same topical antibiotic. If you have had folliculitis return more than twice after treatment, seek a dermatology assessment rather than repeating the same over-the-counter protocol.
Q: Is there a folliculitis treatment available at TTE Elephant without needing a prescription?
A: For mild bacterial folliculitis, TTE's chlorhexidine-based scalp treatment protocol does not require a prescription and can be initiated at first consultation following trichoscopy assessment. This is appropriate for early, non-spreading, non-tender pustules without systemic symptoms. For moderate or severe folliculitis, or any case with spreading or recurrence, TTE will facilitate dermatology referral and coordinate the clinical handover. Prescription antibiotics — topical or oral — require a dermatologist's prescription in Malaysia and are not dispensed at TTE.

