A pimple on the scalp and a pimple on the face look similar, but the scalp's anatomy — dense follicular concentration, occlusion from hair, and a warm, humid microenvironment — makes the differentiation between comedonal acne and bacterial folliculitis critically important. The two conditions share a visual appearance but diverge completely in cause, progression, and treatment. Applying the wrong protocol not only fails to resolve the lesion but frequently worsens it.
In Malaysia's tropical climate, both conditions are more prevalent than in temperate populations. Persistent heat, high ambient humidity, sebum liquefaction at elevated temperatures, and the widespread use of occlusive styling products create ideal conditions for follicular occlusion. Add the mechanical and thermal microenvironment created by hijab wearing, and the incidence of scalp pimples among Malaysian women rises further.
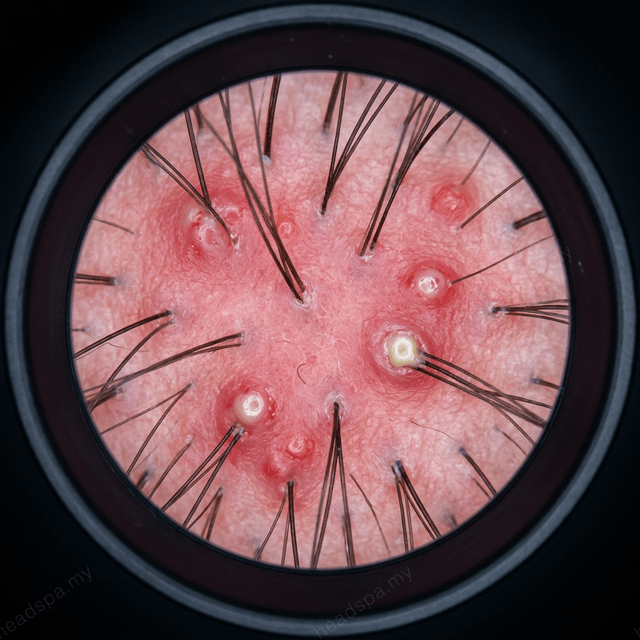
Two Types, Two Mechanisms
| Feature | Comedonal Scalp Acne | Inflammatory Folliculitis | |---|---|---| | Primary cause | Sebum + dead skin cells + product residue forming a plug | Bacterial infection — primarily *Staphylococcus aureus* | | Lesion appearance | Closed whitehead or open blackhead; not pus-filled | Pus-filled pustule; erythematous papule; painful to touch | | Pain level | Minimal to none unless secondarily infected | Tender, throbbing; surrounding erythema | | Distribution | Follows areas of highest sebum output (crown, hairline) | Can appear anywhere; clusters at sites of friction or occlusion | | Progression | Stable unless secondarily infected | Can spread, form furuncles, or progress to scarring | | Malaysian amplifier | Heat + product buildup + high sebum output | Humid microclimate, shared tools, tight hairstyles, hijab occlusion | | Primary treatment | Salicylic acid exfoliation; sebum regulation | Topical antibacterial; chlorhexidine wash; oral antibiotics for severe cases | | Head spa role | Scalp detox, follicle decongestion, sebum regulation | Mild: chlorhexidine protocol + trichoscopy monitoring; moderate-severe: dermatologist referral |
Comedonal Scalp Acne: The Occlusion Pathway
Comedones form when the follicular infundibulum (the opening of the hair follicle at the scalp surface) becomes blocked by a combination of excess sebum, desquamated corneocytes (dead skin cells), and product residues. The plug is not infected — it is mechanical. In Malaysia's heat, sebum is more fluid, spreads further across the scalp surface, and has greater capacity to mix with product residue and dead cells before the follicle can clear it.
Silicone-based conditioners, heavy pomades, and wax-based styling products are frequent contributors. These ingredients are designed for the hair shaft — not the scalp — and repeated application without adequate clarifying creates a progressive layer of residue that narrows the follicular opening over weeks to months.
Comedonal scalp acne responds well to clinical scalp detox protocols incorporating salicylic acid (a beta-hydroxy acid that is oil-soluble and can penetrate the sebum plug) and enzymatic exfoliation. TTE Elephant's trichoscopy assessment confirms the presence of follicular casts and comedonal patterns before initiating treatment, distinguishing this from the bacterial picture that requires an entirely different approach.
Bacterial Folliculitis: The Infection Pathway
Bacterial scalp folliculitis — infection of the hair follicle with *Staphylococcus aureus* or, less commonly, gram-negative organisms — produces a distinctly different clinical picture: painful, erythematous (red) papules and pustules that develop rapidly, are tender on palpation, and may form crusts as they resolve. Unlike comedones, these lesions are not the product of physical occlusion alone. They represent an active infection within the follicle.
Malaysia's climate accelerates folliculitis risk through multiple pathways. Persistent heat and humidity favour bacterial proliferation. Sweating increases skin surface moisture, creating conditions in which *S. aureus* — which colonises the anterior nares and skin of a significant proportion of healthy adults — can more easily invade compromised follicles. Tight hairstyles or braiding create tension at the follicle base, producing micro-trauma that serves as an infection entry point.
The Hijab Microenvironment
For Muslimah clients, the scalp microenvironment beneath a hijab warrants particular clinical attention. Covered scalp skin maintains higher temperature and relative humidity than exposed skin, creating conditions that measurably favour both Malassezia overgrowth (associated with seborrhoeic dermatitis and pityrosporum folliculitis) and bacterial folliculitis. Friction from fabric along the hairline and neck amplifies mechanical follicular trauma.
This is not a reason to avoid wearing hijab — it is a reason to implement a structured scalp hygiene and treatment protocol designed around that specific microenvironment. TTE's team includes therapists trained to provide clinical guidance for Muslimah scalp health specifically, including compatible treatment protocols and product recommendations. Our [KL clinic](/headspa-kl) and [JB clinic](/headspa-jb) are fully equipped to assess and manage these cases.
Treatment Decision Framework
For mild comedonal scalp acne without infection signs, clinical head spa treatment is appropriate as a primary intervention: professional scalp detox, sebum normalisation, and product residue removal combined with guidance on cleansing frequency and product selection.
For suspected bacterial folliculitis, the first step is correct identification. Pustular lesions, pain, and erythema signal infection, and topical antibacterial agents (mupirocin, clindamycin) or chlorhexidine-based scalp washes are indicated. TTE's protocol includes trichoscopy-guided identification and can manage mild folliculitis with a chlorhexidine scalp treatment protocol. Moderate to severe folliculitis — widespread pustules, furuncle formation, or lesions not resolving within two weeks — requires dermatologist referral for systemic antibiotic consideration and to rule out antibiotic-resistant strains.
When to refer to a dermatologist immediately: lesions spreading rapidly, fever, associated lymphadenopathy, furuncle formation, or any folliculitis in an immunocompromised individual.
Related reading: [Scalp Folliculitis Symptom Profile](/concerns/scalp-folliculitis) | [TTE Elephant Head Spa KL](/headspa-kl) | [TTE Elephant Head Spa JB](/headspa-jb)
---
Frequently Asked Questions
Q: How do I know if the pimples on my scalp are infected or just clogged?
A: The key distinguishing features are pain, colour, and content. A comedone (clogged follicle) is typically non-painful, skin-coloured or slightly whitish, and does not contain visible pus. Bacterial folliculitis produces a clearly pus-filled pustule surrounded by a red halo, is tender to the touch, and may feel warm. If you are uncertain, a trichoscopy assessment at TTE will differentiate the two within the first consultation.
Q: Can wearing a hijab cause scalp pimples?
A: Not directly, but the microenvironment beneath a hijab — elevated temperature, higher humidity, and friction at the hairline — creates conditions that amplify both comedonal acne and bacterial folliculitis risk. A well-designed scalp hygiene protocol, appropriate fabric selection, and regular clinical assessment can manage this effectively. TTE Elephant offers consultation specifically for Muslimah scalp concerns.
Q: Is it safe to have a head spa treatment when I have scalp pimples?
A: It depends on the type and severity. Comedonal scalp acne is well-suited to clinical head spa treatment — scalp detox and professional exfoliation are core interventions. Active bacterial folliculitis requires assessment first; mild cases can proceed with a modified antibacterial protocol, while moderate to severe infection is referred to a dermatologist before spa treatment resumes. Do not undergo any mechanical scalp massage over active, pus-filled pustules without clinical clearance.
Q: Will salicylic acid shampoo fix scalp pimples?
A: For comedonal acne, salicylic acid at 1–2% concentration is an appropriate keratolytic that helps break down the sebum-cell plug in the follicle. For bacterial folliculitis, salicylic acid has no antibacterial action and will not resolve the infection. Applying it to pustular folliculitis may reduce surface scale but leaves the underlying infection untreated, allowing progression to more severe stages.

